BRIAN ONGORO
World's First Malaria Vaccine Offers Hope to Millions
Tens of thousands of lives could be saved each year from sickness and death caused by malaria following the World Health Organization (WHO) approval of a first-ever vaccine. Scientists have recommended the RTS,S vaccine for children in sub-Saharan Africa and other high-risk areas to prevent one of the world’s oldest and deadliest infectious diseases.
Malaria causes around 400,000 deaths worldwide each year, killing more than 625,000 in 2020 as the COVID-19 pandemic and Ebola outbreaks made treatment more difficult. More than half of all deaths annually are African children under the age of five whose immune systems are more vulnerable to severe malaria.
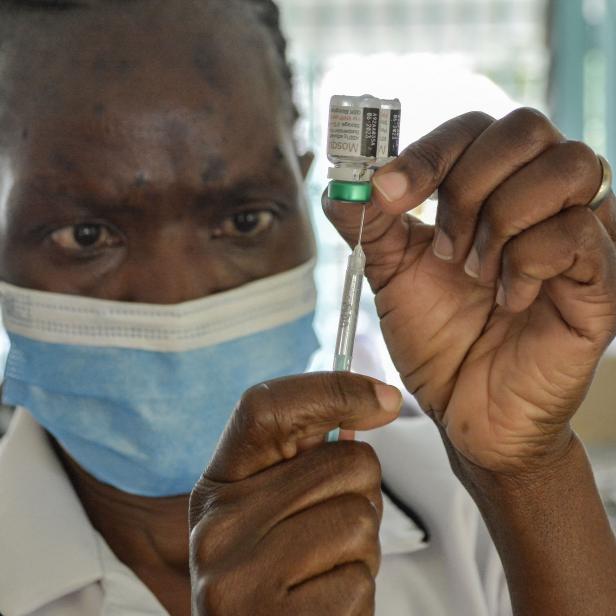
Health agencies keep cases down with drugs and by giving out insecticide-laced bed nets, which kill mosquitoes that spread the malarial parasite. But WHO director-general Dr. Tedros Ghebreyesus said the extra protection from RTS,S vaccine, or Mosquirix, is “a historic moment” for health and malaria control.
More than 90 percent of the world’s deaths occur in malaria-endemic countries across sub-Saharan Africa. So the WHO’s vaccine pilot programs have targeted 800,000 children across Ghana, Kenya, and Malawi since 2019. Four doses are given to children from five months of age. Mosquirix acts against the most deadly malaria parasite (Plasmodium falciparum) transmitted by the bite of a female mosquito.
BRIAN ONGORO
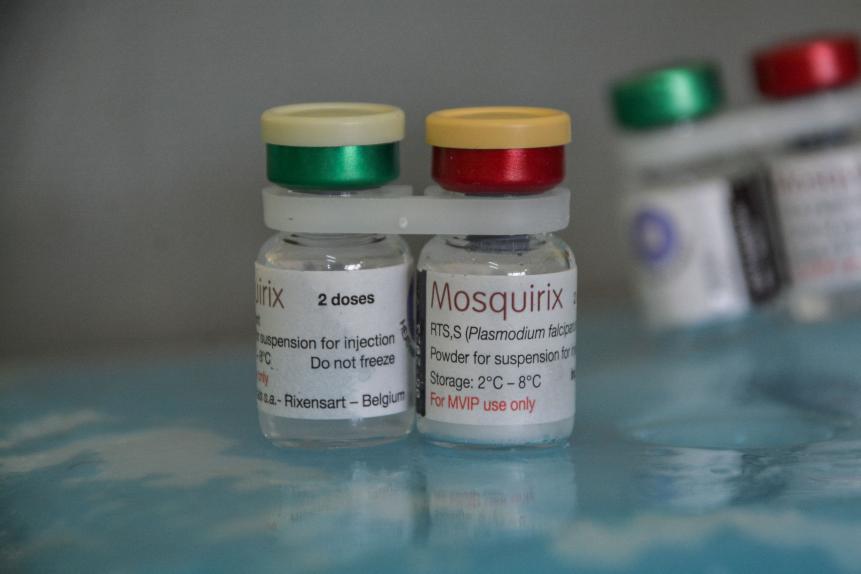
World Health Organization approved using the malaria vaccine, Mosquirix, on children between 5-month to 5-year old in sub-Saharan Africa and other parts with moderate to high malaria transmission after the malaria vaccine implementation program (MVIP) in Ghana, Kenya, and Malawi.
Severe malaria is almost always caused by Plasmodium falciparum. Infections can rapidly lead to complications and death without the right treatment. Symptoms include fever and chills followed by breathing problems, anemia, seizures, brain damage, and coma for more severe cases.
Modeling for countries with the highest reported malaria cases predicts the vaccine could prevent 5.3 million cases and 24,000 deaths yearly in children younger than five. So far, the actual numbers are encouraging, with 2.3 million doses given and a 30 percent reduction in deadly severe malaria, even in areas where bed nets are used and good drug treatment is available.
WHO’s regional director for Africa, Dr. Matshidiso Moeti said the vaccine “offers a glimmer of hope for the continent which shoulders the heaviest burden of the disease, and we expect many more African children to be protected from malaria and grow into healthy adults.”
BRIAN ONGORO
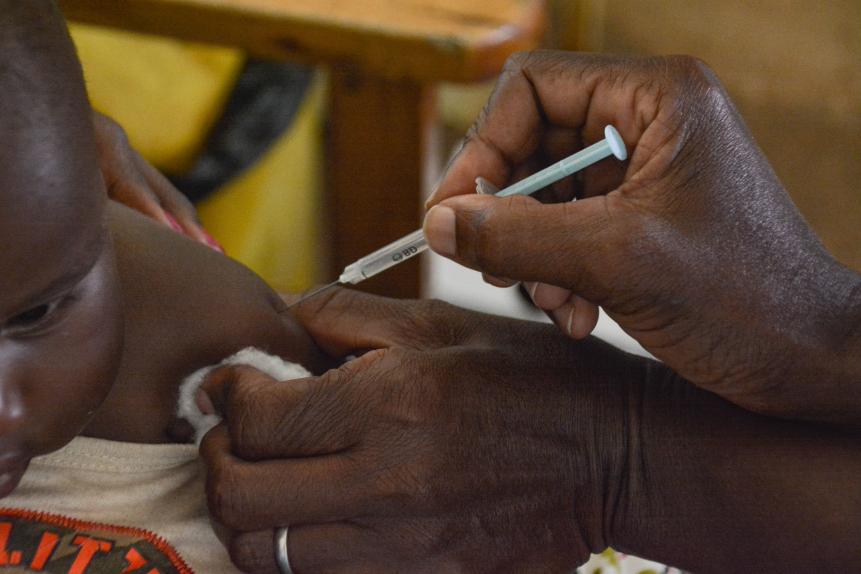
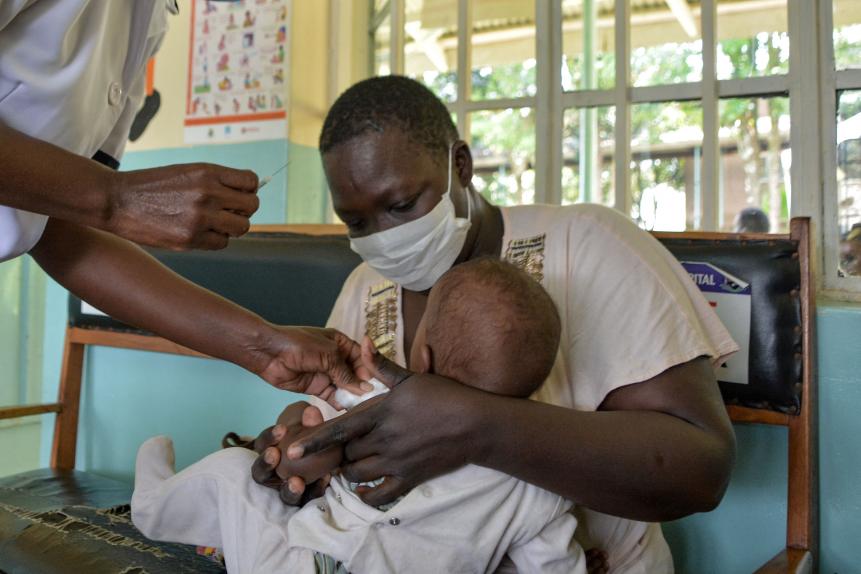
A child gets a malaria vaccination at Yala Sub-County hospital, in Yala, Kenya, on October 7, 2021.
One trial showed that given together with anti-malarial drugs the vaccine was 70 percent effective against hospitalization with severe malaria and 75 percent effective in preventing death.
The WHO’s strategy is to reduce global malaria cases and deaths by at least 90 percent by 2030. And that could boost health generally because malaria can repeatedly affect people time and again, leaving their immune system compromised and open to other diseases.
New generations of malaria vaccines use RNA technology to trigger an immune response – like the successful COVID-19 vaccines – and that could help the WHO reach its target with time to spare. Yale University is working with the pharmaceutical industry to create a self-amplifying RNA (saRNA) vaccine that could be rapidly scaled to produce billions of doses.
Pieces of saRNA contain instructions that disrupt a protein used by the parasite to stop the body from producing memory T-cells for immunity. By attacking this protein, called PMIF, the vaccine allows the body to defend itself naturally and generate long-term protection against malaria. The RNA is also coded to copy itself inside the body, meaning much smaller amounts can be injected to fight the disease.
BRIAN ONGORO
A family prepares to receive Malaria vaccinations in Kenya.
Another RNA vaccine under development from BioNTech uses messenger RNA (mRNA) to target the circumsporozoite protein (CSP) – the same protein targeted by RTS,S. BioNTech’s mRNA vaccine tells the body to make CSP and that triggers an immune response, which can destroy the parasite once it is transmitted by a mosquito bite.
The promise of mRNA/RNA as a vaccine agent is definitely gathering pace. Using mRNA vaccines to protect people against SARS-CoV-2 has proved its effectiveness. Now there are shots in development for HIV, cancer, and flu as well as malaria.